The prostate cancer treatment that’s right for you depends on several factors, including your age, the Gleason score, the cancer's stage, your symptoms, and your general health. Because prostate cancer typically grows slowly, most men have time to review their treatment options and consider the pros and cons of a few different treatment paths. Your oncologist will determine how likely your cancer is to grow and spread beyond the prostate as part of the treatment planning process.
Prostate Cancer Treatment Options
Although a common approach, prostate cancer removal surgery is not always a necessary part of treatment. Men with the earliest stages of prostate cancer may be recommended an active surveillance approach before beginning other treatments.
Prostate cancer patients may receive one or a combination of the following treatments, including:
Determining the Right Treatment Plan for Each Patient
Prostate cancer doctors consider the individual’s risk of localized cancer growing outside of the prostate when selecting a treatment plan. The more likely cancer is to grow and spread, the sooner treatment will need to begin.
Prostate Cancer Risk Groups
Risk groups are categorized into three general groups based on the patient's prostate-specific antigen (PSA), digital rectal exam (DRE), and biopsy results. These groups include:
Low-risk: Prostate cancers in the low-risk group are small, confined to the prostate, and have a low grade. This means the cancer is growing slowly. They also have a low PSA level (less than 10). These cancers rarely cause any symptoms and are not likely to grow outside of the prostate. Tumors that are undetectable by a digital rectal exam or show no sign of cancer in two previous biopsies fall into a subset called "very low risk.
Intermediate-risk: Prostate cancer tumors in this category are confined to the prostate, but the PSA level is higher (between 10 and 20). The grade is also higher than low-risk prostate cancer. This means the grade group is a 2 or a 3, and cancer cells are actively growing. Intermediate risk is often divided into "favorable" – slower spread, and "unfavorable" – more likely to spread quicker.
High-risk: High-risk groups indicate that the tumor has extended outside the prostate, the PSA is greater than 20, and the grade group is higher (4 or 5). Tumors that have extended into the seminal vesicles, rectum, or bladder, or have had multiple biopsy samples with high-grade cancer, fall into a subset of very aggressive tumors called "very high risk."
The prostate cancer oncologist uses these risk groups to consider the treatments and their timing. For example, low-risk patients will likely go into active surveillance, while high-risk patients will be more likely to start one or more treatments right away.
Lab Tests Used for Planning Prostate Cancer Treatment
Our oncologists also use special lab tests, such as genomic, molecular, or proteomic tests, to predict how quickly the cancer might grow, such as:
ProMark: This test measures the activity of a set of proteins in prostate cancer cells taken from a biopsy and provides a score that predicts the likelihood of the cancer growing and spreading quickly.
Oncotype DX Prostate: This test tracks certain genes in cancer cells taken from a biopsy and reports a score on a scale from 0 to 100. Higher scores indicate a cancer that is more likely to grow and spread quickly and has a higher risk of causing death from prostate cancer.
Decipher: This test measures the activity of certain genes in prostate cancer cells taken from a biopsy and creates a risk score on a scale from 0 to 1. A higher score means a higher likelihood of the cancer spreading beyond the prostate. For men undergoing surgery (prostatectomy) to treat their cancer, a similar test can be used to measure the activity of certain genes in prostate cancer cells from the surgery tissue. This can help determine the risk of the cancer recurring in other parts of the body after surgery and whether further treatment should be considered.
Prolaris: This test tracks a different set of genes in prostate cancer cells taken from a biopsy and provides a score on a scale from 0 to 10. A higher score indicates a cancer that is more likely to grow and spread quickly and has a higher risk of causing death from prostate cancer.
Be sure to talk with your oncologist about what to expect from these tests, including their accuracy and how they will use the information provided by the test results.
Active Surveillance
You may choose active surveillance if the risks and possible side effects of treatment outweigh the possible benefits. Your doctor may suggest active surveillance if you’re diagnosed with early-stage prostate cancer that seems to be slowly growing. Your doctor may also offer this option if you are older or have other serious health problems.
Choosing active surveillance doesn’t mean you’re giving up. It means you’re putting off the side effects of surgery or radiation therapy. Having surgery or radiation therapy is no guarantee that a man will live longer than a man who chooses to put off treatment.
If you and your doctor agree that active surveillance is a good idea, your doctor will check you regularly (such as every 3 to 6 months, at first). After about one year, your doctor may order another biopsy to check the Gleason score. You may begin treatment if your Gleason score rises, your PSA level starts to rise, or you develop symptoms. You’ll receive surgery, radiation therapy, or another approach.
Active surveillance avoids or delays the side effects of surgery and radiation therapy, but this choice has risks. For some men, it may reduce the chance of controlling cancer before it spreads. Also, it may be harder to cope with surgery or radiation therapy when you’re older.
If you choose active surveillance but grow concerned later, you should discuss your feelings with your doctor. Another approach is an option for most men.

Radiation Therapy for Prostate Cancer Treatment
Radiation therapy is an option for men with any stage of prostate cancer. Men with early-stage prostate cancer may choose radiation therapy instead of surgery. It may also be used after surgery to destroy any cancer cells that remain in the area. In later stages of prostate cancer, radiation treatment may be used to help relieve pain.
Radiation therapy (also called radiotherapy) uses high-energy rays to kill cancer cells. It affects cells only in the treated area.
Doctors use two types of radiation therapy to treat prostate cancer: external beam radiation and internal radiation. Some men receive both types.
External Beam Radiation
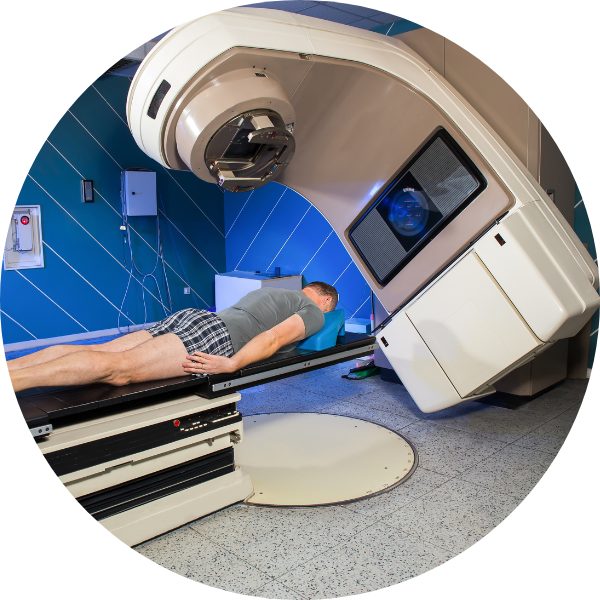
During these short treatment sessions, you lie down on a table, and a linear accelerator machine is directed to the exact spot where the cancer is located. The beams of radiation are then delivered from the linear accelerator.
Many men receive 3-dimensional conformal radiation therapy or intensity-modulated radiation therapy. These types of treatment use computers to more closely target the cancer to lessen the damage to healthy tissue near the prostate.
The length of time that each patient receives radiation therapy depends on several things, including the stage of cancer. Traditionally, this would be completed in 6-8 weeks. With a more advanced approach, called hypofractionated radiation therapy, the same dose of radiation can be given in each session, reducing the total number of weeks that treatments are needed. Hypofractionated radiation therapy usually lasts only 4-5 weeks.
The specific number of treatment sessions will depend on the exact location of the cancer, its size, and the overall health condition.
Internal Radiation (Implant Radiation or Brachytherapy)
The radiation comes from radioactive material, usually contained in very small implants called seeds. Dozens of seeds are placed inside needles, and the needles are inserted into the prostate. The needles are removed, leaving the seeds behind. The seeds give off radiation for months. They don’t need to be removed once the radiation is gone. Read our blog to find out what you should know about internal radiation for prostate cancer treatment.
Side Effects of Radiation Therapy
Both internal and external radiation can cause impotence. For most men, this improves after radiation therapy is complete. You can talk with your doctor about ways to help cope with this side effect. Other side effects can include fatigue and diarrhea. Talk with your prostate cancer specialist about ways to prepare for and manage the side effects of radiation therapy.
Affiliated Oncologists offers radiation therapy for prostate cancer treatment in the suburbs of South Chicago so that it’s convenient for local residents to receive this type of cancer treatment.
Hormone Therapy for Prostate Cancer
A man with prostate cancer may have hormone therapy before, during, or after radiation therapy. Hormone therapy is also used alone for prostate cancer that has returned after treatment.
Male hormones (androgens) can cause prostate cancer to grow. Hormone therapy keeps prostate cancer cells from getting the male hormones they need to grow. The testicles are the body’s main source of the male hormone testosterone. The adrenal gland makes other male hormones and a small amount of testosterone.
Hormone therapy uses drugs or surgery:
- Drugs: Your doctor may suggest a drug that can block natural hormones:
- Luteinizing hormone-releasing hormone (LH-RH) agonists: These drugs can prevent the testicles from making testosterone. Examples are leuprolide, goserelin, and triptorelin. The testosterone level falls slowly. Without testosterone, the tumor shrinks, or its growth slows. These drugs are also called gonadotropin-releasing hormone (GnRH) agonists.
- Antiandrogens: These drugs can block the action of male hormones. Examples are flutamide, bicalutamide, and nilutamide.
- Other drugs: Some drugs can prevent the adrenal gland from making testosterone. Examples are ketoconazole and aminoglutethimide.
- Surgery: Surgery to remove the testicles is called orchiectomy.
Doctors usually treat prostate cancer that has spread to other parts of the body with hormone therapy. For some men, the cancer will be controlled for two or three years, but others will have a much shorter response to hormone therapy. In time, most prostate cancers can grow with very little or no male hormones, and hormone therapy alone is no longer helpful. At that time, your doctor may suggest chemotherapy or other forms of treatment that are under study. In many cases, the doctor may suggest continuing with hormone therapy because it may still be effective against some of the cancer cells.
Radiopharmaceuticals for Advanced Prostate Cancer
Affiliated Oncologists offer men with metastatic, castration-resistant prostate cancer (mCRPC) — a challenging and advanced stage of the disease — access to a groundbreaking treatment. This innovative approach combines diagnostic imaging with Pluvicto™, a radiopharmaceutical approved by the US Food and Drug Administration, designed to specifically target and destroy prostate cancer cells.
What Can Advanced Prostate Cancer Patients Expect?
Patients who qualify for this treatment will first undergo a PET scan using a tracer called Pylarify®. This tracer attaches to prostate-specific membrane antigens found on some prostate cancer cells, providing a more precise image of the tumor(s) compared to traditional imaging technologies.
After imaging, eligible patients will begin treatment with Pluvicto™. This unique therapy is designed to identify and bind to the prostate-specific membrane antigen (PSMA) protein on prostate cancer cells. It then emits radiation to destroy the cancer cells while leaving healthy tissue unharmed. Several treatments are given over 6 to 9 months.
The combination of Pylarify® imaging and Pluvicto™ therapy gives new hope to men whose cancer has spread or become resistant to other treatments. Clinical trials have shown that this therapy can extend survival for patients with metastatic castration-resistant prostate cancer.
Surgery to Remove the Prostate
Surgery is an option for men with early (Stage I or II) prostate cancer. It’s sometimes an option for men with Stage III or IV prostate cancer. The surgeon may remove the whole prostate or only part of it.
Before the surgeon removes the prostate, the lymph nodes in the pelvis may be removed. If prostate cancer cells are found in the lymph nodes, the disease may have spread to other parts of the body. If cancer has spread to the lymph nodes, the surgeon does not always remove the prostate and may suggest other types of treatment.
There are several types of surgery for prostate cancer. Each type has benefits and risks. You and your doctor can talk about the types of surgery and which may be right for you:
- Open surgery: The surgeon makes a large incision (cut) into your body to remove the tumor. There are two approaches:
Through the abdomen: The surgeon removes the entire prostate through a cut in the abdomen. This is called a radical retropubic prostatectomy.
Between the scrotum and anus: The surgeon removes the entire prostate through a cut between the scrotum and the anus. This is called a radical perineal prostatectomy.
Laparoscopic prostatectomy: The surgeon removes the entire prostate through small cuts, rather than a single long cut in the abdomen. A thin, lighted tube (a laparoscope) helps the surgeon remove the prostate.
Robotic laparoscopic surgery: The surgeon removes the entire prostate through small cuts. A laparoscope and a robot are used to help remove the prostate. The surgeon uses handles below a computer display to control the robot’s arms.
Cryosurgery: For some men, cryosurgery is an option. The surgeon inserts a tool through a small cut between the scrotum and anus. The tool freezes and kills prostate tissue.
TURP: A man with advanced prostate cancer may choose TURP (transurethral resection of the prostate) to relieve symptoms. The surgeon inserts a long, thin scope through the urethra. A cutting tool at the end of the scope removes tissue from the inside of the prostate. TURP may not remove all of the cancer, but it can remove tissue that blocks the flow of urine.
Surgery can damage the nerves around the prostate. Damaging these nerves can make a man impotent (unable to have an erection). In some cases, your surgeon can protect the nerves that control erection. But if you have a large tumor or a tumor that’s very close to the nerves, surgery may cause impotence. Impotence can be permanent. You can talk with your doctor about medicine and other ways to help manage the sexual side effects of cancer treatment.
If your prostate is removed, you will no longer produce semen. You’ll have dry orgasms. If you wish to father children, you may consider sperm banking or a sperm retrieval procedure before surgery.

Prostate Cancer Targeted Therapy
Men with advanced prostate cancer, or those whose tumors have abnormal characteristics, may benefit from targeted therapy as part of their treatment plan.
Targeted therapy involves using medications or other substances to identify and attack specific cancer cells that contain abnormal proteins, receptors, or genes. Unlike chemotherapy, which affects both cancerous and healthy cells, targeted therapy is more precise, resulting in different and generally fewer side effects.
Prostate cancer targeted therapy drugs are known as PARP inhibitors. PARP (poly(ADP)-ribose polymerase) enzymes are proteins inside cells that normally help repair damaged DNA, including the DNA of cancer cells, by blocking the cancer cells' ability to repair themselves. This includes cancerous cells with genetic mutations, such as BRCA1 or BRCA2. PARP inhibitors can also be effective when other DNA repair genes, known as homologous recombinant repair (HRR) genes, are present.
Before starting treatment with a PARP inhibitor, your doctor will likely test your blood or cancer cells to confirm the presence of a DNA repair gene mutation. Targeted therapy for prostate cancer is typically administered as oral pills or capsules, usually taken once or twice a day.
Immunotherapy for Prostate Cancer
Immunotherapy stimulates the body’s immune system to help destroy cancer cells. The use of immunotherapy for prostate cancer shows great promise and potential to change how patients are treated for prostate cancer. There are two main types of immunotherapy used for prostate cancer: cancer vaccines and immune checkpoint inhibitors.
Prostate Cancer Vaccine
Cancer vaccines are emerging as a promising treatment option for advanced prostate cancer that no longer responds to hormone therapy. Each vaccine is tailor-made for the patient. This process involves extracting white blood cells from your blood and mixing them with a protein from prostate cancer cells called prostatic acid phosphatase (PAP). The mixture is then injected back into your body.
Patients will undergo this procedure two more times, at two-week intervals, for a total of three doses. The goal of a cancer vaccine is to help the immune system’s cells target and attack prostate cancer cells.
Sipuleucel-T (Provenge) is an approved cancer vaccine for the treatment of prostate cancer.
While cancer vaccines aren't considered a cure for prostate cancer, they can help slow cancer growth, allowing many men to live longer.
Checkpoint Inhibitors
An immune checkpoint is normally used by the body to regulate the immune response and prevent it from attacking healthy cells. To help target these checkpoints, your oncologist may recommend a type of immunotherapy drug known as a checkpoint inhibitor.
Checkpoint inhibitors may be an option for patients whose tumors show specific genetic traits, such as high levels of microsatellite instability (MSI-H), mismatch repair deficiency (dMMR), or a high tumor mutational burden (TMB-H).
These genetic mutations are less common in prostate cancer compared to other types of cancer, but can significantly influence how well the treatment works. If your doctor recommends immunotherapy as part of your treatment plan, you will receive these drugs as an intravenous (IV) infusion, typically every 3 to 6 weeks.
Research on immunotherapy for prostate cancer is ongoing, particularly regarding combination treatments, such as pairing a checkpoint inhibitor with a prostate cancer vaccine. This approach may strengthen the immune response and improve the effectiveness of the vaccine.
Chemotherapy for Prostate Cancer
Chemotherapy may be used for prostate cancer that has spread and no longer responds to hormone therapy.
Clinical Trials for Prostate Cancer
A clinical trial is a research study meant to help improve current treatments or gather information on new treatment methods for patients with cancer. When clinical trials show that a new treatment is better than the standard treatment, the new treatment may become the standard treatment. The results of the clinical trials we participate in will advance the knowledge and treatments for patients everywhere. Consult with your cancer care team at Affiliated Oncologists to learn more about clinical trials for prostate cancer and if one is right for you.
Prostate Cancer Treatment Available in the South Chicago Area
If you were recently diagnosed with prostate cancer or you are in active surveillance, our cancer care team in the South Chicago suburbs can help you determine the best next steps for you. Our prostate cancer doctors offer the latest prostate cancer treatments available with personalized treatment plans tailored to you. Make an appointment at one of the Affiliated Oncologists locations in Chicago Ridge, Mokena, Hazel Crest, Palos Heights, New Lenox, Orland Park, or Oak Lawn, IL to consult with our prostate cancer specialists.